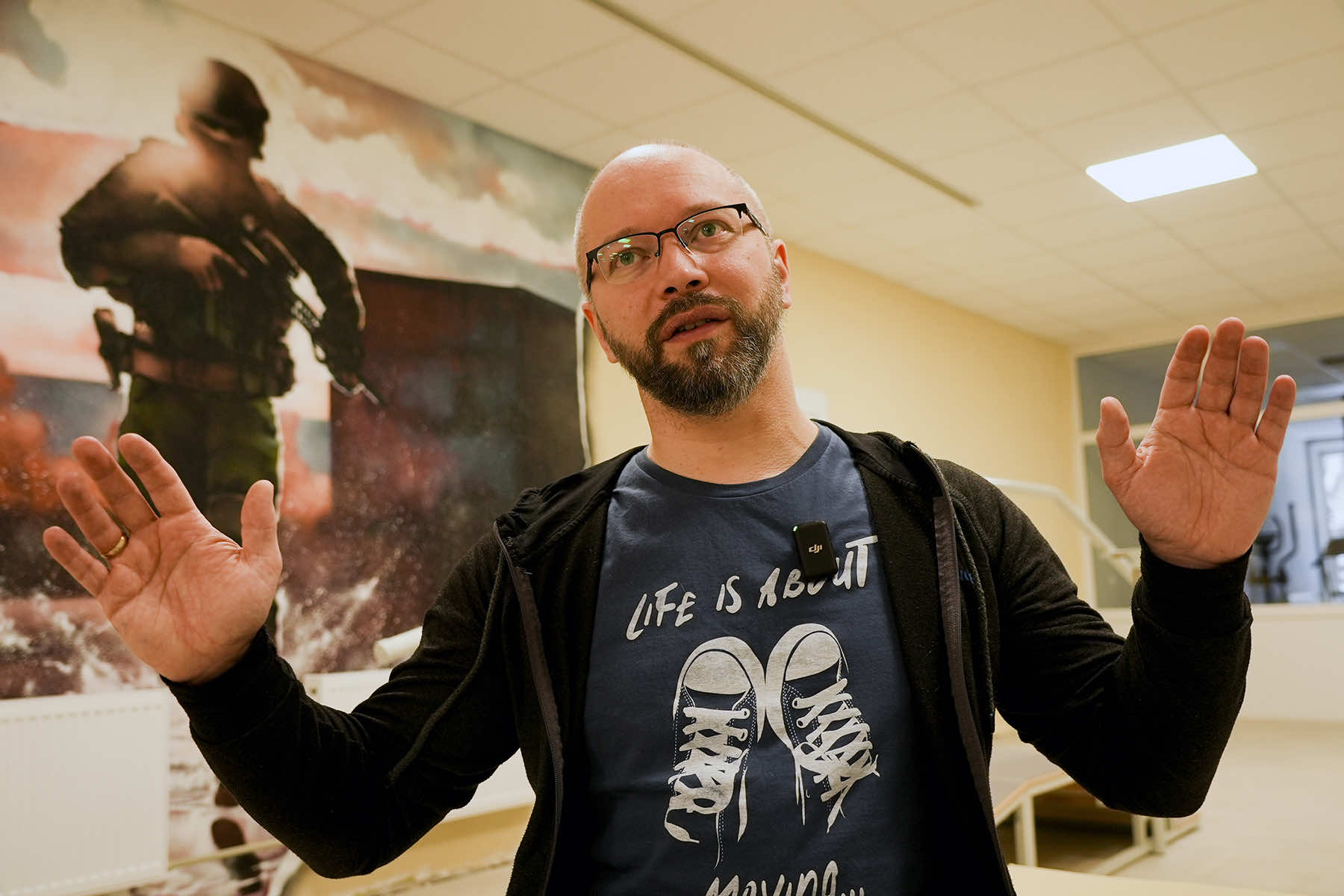Sleep plunges the soldier back into the horrors of Ukraine’s battlefields. He can hear bombs falling again and picture explosions. He imagines himself frantically running, trying to save himself and others.
The nightmares are so vivid and frightening that he pleads with his doctor for help. “It will blow my mind,” he warns. “So do something.”
“Very, very, very stressful,” Witalij Miskow, 45, says of the night terrors he is fighting with tranquilizers and therapy at a mental health treatment center for soldiers on the outskirts of Ukraine’s capital, Kyiv.
When peace eventually returns to Ukraine, many thousands of other soldiers are likely to come home like Miskow with a condition known as post-traumatic stress disorder, or PTSD. Psychologists, veterans affairs officers and former combatants who have struggled with nightmares, distressing flashbacks and other PTSD symptoms are already working to head off a potential mental health crisis among soldiers and their families from the particularly gruesome, intense and grinding war.
Whether it is increasing awareness and funding for mental health care or training counsellors to help soldiers talk through psychological traumas, the goal is to prevent potentially destructive PTSD-related problems, including suicides, family violence, alcohol and drug abuse, from taking root.
Ex-paratrooper Sgt. Maksym Pasichnyk says civilian life was “very complex” for him after years of fighting pro-Russian forces in eastern Ukraine and once Moscow then launched its full-blown invasion, now in its tenth month. His long exposure to combat, death and destruction left the 28-year-old with an array of PTSD symptoms. He fears many other servicemen and their families could likewise suffer.
“The repercussions come later. You have a din in your ears, you start vomiting, you come home and have constant shifts of blood pressure and you lash out at your family members, your kids, your wife,” he says.
“You constantly think that someone is watching you, you overthink, you abuse drugs and drink, you lose yourself,” he adds. “If you want to get help, you are interned in a psychiatric hospital, where they turn you into a vegetable. If you show flashes of anger, they give you tranquilizers and you just sit there.”
Pasichnyk saw his last combat at the very start of the February 24 invasion. His unit was inserted by helicopter at night to defend an airfield on Kyiv’s outskirts. The firefights and ensuing long slog back to the capital butchered his feet. The bleeding, bruising and bone fractures were so severe that he was discharged from further service.
Outwardly, the muscular veteran looks a picture of health. But physical integrity can hide soldiers’ inner suffering, Pasichnyk cautions.
“They look fine,” he says, “but they’re not.”
On November 12, Pasichnyk went back to the damaged Hostomel airbase where he fought, a return that again stirred flashbacks of the events he endured there. Setting off from the disemboweled remains of what before the battle had been the world’s biggest aircraft, he ran a half-marathon to raise awareness of PTSD and to fund the treatment costs for 10 veterans with symptoms.
Pasichnyk says he worries not only about the risk of traumatized soldiers taking their own lives but also that they could turn guns on others and “might resort to terrorist acts.”
Ukraine’s Veterans Affairs Ministry spokeswoman Iulia Vorona says statistics on suicides and PTSD among veterans and their families aren’t being made public during the war for security reasons.
But speaking five months before the invasion, the veterans affairs minister, Yuliia Laputina, said there had already been “great demand” from military families for psychological support as a result of fighting since 2014 against Moscow-backed separatists in eastern Ukraine.
The minister, who has a Ph.D. in psychology, expressed particular concern that many are going back to “remote villages where there is no psychologist.”
“We must build a system where emergency psychological assistance will work in the most remote corners,” she said.
In a subsequent interview this month with The Associated Press, one of her deputies, Eugen Kotyk, said the ministry is “actively working” on a suicide and alcohol risk-reduction program.
Based on figures from previous conflicts, around 20% of troops exposed to intense fighting in Ukraine could develop PTSD, estimates British psychiatrist Neil Greenberg, a professor of defense mental health at King’s College university in London who previously served as a Royal Navy medical officer for 23 years, including in Iraq and Afghanistan. In the wake of the Russian invasion, he has also done online training for the Ukrainian military on managing traumatic events.
Unlike soldiers who fought in Afghanistan or U.S. troops in the Vietnam war, Ukrainian soldiers are fighting in and for their homeland, with evident public support, a clear enemy and solid goals and justifications. All that could help lessen the mental heath fallout for Ukrainian veterans, says Greenberg, who describes it as “a psychologically good war for Ukraine.”
But a victory for Ukraine, returning soldiers being well-treated afterward and reconstruction will also play roles in determining whether psychological illnesses cause “mass, mass casualties” among veterans “or just a large number,” Greenberg adds.
Anticipating that many will need help, Ukrainian psychologist Andrii Omelchenko is training volunteers — 300 so far and aiming for a total of 2,000 — to provide counselling to soldiers.
Omelchenko also does hands-on counselling with troops in the field and continues that work online when he is back in Kyiv, talking them through battlefield traumas on video calls from his 17th-floor office. One recent call was with a frontline commander who was suffering from debilitating panic attacks, after he’d seen a missile strike that severely injured three soldiers.
Russia’s heavy reliance on artillery bombardments is exacting a psychological toll on Ukrainian solders, Omelchenko says. He says social media are another psychological stress because they show soldiers that while they’re in trenches, loved ones and friends may be enjoying comparatively normal lives.
“It’s really painful,” Omelchenko says. “Civilian life has a lot of good things which are not proper to show.”
On the other hand, Omelchenko says he is also fielding calls from families asking how best to deal with soldiers who are coming back changed from battle — taciturn, distant, on edge and in their own worlds. Omelchenko previously experienced that himself with his grandfather, who’d fought as a young teenager in World War II.
“My grandfather never smiled,” Omelchenko says.
At the Forest Glade rehabilitation clinic outside Kyiv, Miskow is continuing his recovery. As well as pharmaceuticals, the facility uses yoga, acupuncture, soothing sounds and other therapies on its 220 patients.
“I’m happy, I’m still alive,” Miskow says.
Still, he then cries when talking about an artillery strike that killed several of his friends.
“I’m getting used (to) these feelings, but it’s still very, very difficult,” he says. “If you’re not here, you don’t understand at all, you won’t understand.”